Rita Agarwal MD, FAAP, FASA
If it feels like practicing medicine and anesthesiology has gotten harder over the past few years, that’s because it has.
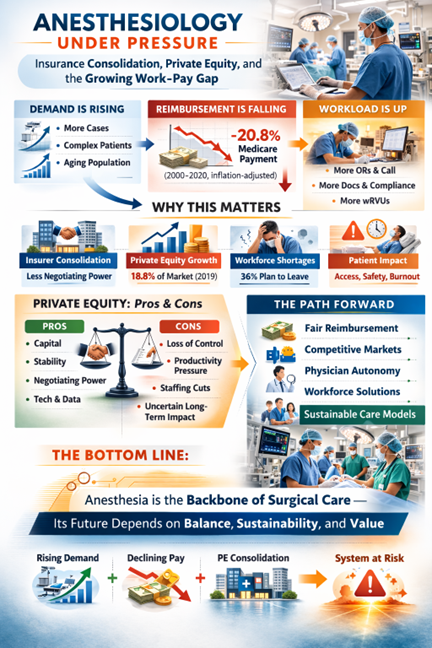
Many of us are seeing more patients, generating more work, and navigating increasingly complex administrative demands — and taking home less or the same as we were 2 years ago. Several forces are quietly reshaping the landscape of physician practice: health insurance consolidation, rapid expansion of private equity, and a widening gap between physician productivity and compensation.
These are not abstract policy issues. They affect our practices, our patients, and our professional sustainability.
Demand Is Rising. Reimbursement Is Not.
The demand for anesthesia services continues to grow:
- The U.S. population aged 65 and older is projected to increase by 55% by 2030.
- Procedural volume is expected to rise in the coming decade.
- Workforce shortages persist.
At the same time, inflation-adjusted Medicare payment per anesthesia service declined 20.8% between 2000 and 2020.
This creates a structural imbalance:
Rising demand + Declining real reimbursement = Growing pressure on anesthesiology.
Hospitals are increasingly offsetting this gap through stipends. In some states, more than half of hospitals now provide financial support to anesthesia groups. While stipends stabilize coverage in the short term, they signal a fragile underlying reimbursement model.
When Insurers Get Bigger, Leverage Gets Smaller
In many metropolitan markets, one or two insurers control the majority of commercial contracts.
When competition shrinks:
- Negotiating power declines
- Reimbursement rates decrease
- Administrative burdens increase
- Independent practice becomes harder to sustain
For anesthesiologists, the challenge is amplified. As facility-based physicians, we rarely control payer mix and cannot easily exit dominant contracts without jeopardizing hospital relationships.
Negotiations increasingly feel less like negotiations—and more like ultimatums. ”Take it or Leave it”
Lower reimbursement limits investment in:
- Staffing
- Technology
- Infrastructure
- Recruitment
Over time, this accelerates burnout and consolidation
Working More, Earning Less
National data show that physician productivity has increased significantly in recent years. Measured in wRVUs, physicians are delivering more care than ever 2.
In anesthesiology, this often means:
- Higher room concurrency
- More add-on cases
- Sicker patients
- Longer hours, more days worked
- Increased call coverage
- Expanded non-OR anesthesia
- Greater documentation requirements
Meanwhile, labor now represents more than 80% of physician practice operating costs. As staffing costs rise and reimbursement remains constrained, margins tighten.
The practical result:
We are generating more clinical work —
but the return per unit of work is shrinking.
The Rise of Private Equity in Anesthesia
Against this backdrop of payer consolidation and financial pressure, private equity (PE) has rapidly expanded in anesthesiology3.
Key trends:
- Private equity investment in healthcare exceeded $200 billion in 2021.
- Nearly one in five anesthesia practices were under PE management by 2019.
- Anesthesiologists represent a significant portion of PE-acquired physicians.
Private equity firms often acquire practices using “roll-up” strategies—aggregating smaller groups into large regional or national entities.
Why anesthesia?
- Predictable procedural demand
- Fragmented independent groups
- Workforce shortages that increase negotiating leverage
- Hospitals that are significantly larger than typical anesthesia practices
For some groups, PE offers capital, infrastructure support, and short-term financial stability.
The Benefits — and the Trade-Offs
Private equity partnerships may provide:
- Immediate capital infusion
- Improved revenue cycle billing management
- Data analytics and benchmarking
- Greater negotiating leverage
- Relief from administrative burdens
- Reimbursement rates may improve following consolidation.
However, ownership transitions often shift anesthesiologists from equity partners to employees. That shift can bring:
- Reduced governance control
- Increased productivity targets
- Operational efficiency mandates
- Cultural change within groups
- Mixed effects on staffing, turnover and quality
The long-term impact remains uncertain.
Private equity typically operates on a 3–7 year investment horizon. Anesthesiology, by contrast, depends on long-term workforce stability, investment in training, and a culture of patient safety.
These Forces Are Connected
Insurance consolidation, the rise in PE and the work–pay gap are not separate phenomena. They are deeply intertwined.
When dominant insurers push down reimbursement rates, health systems receive less revenue per encounter. To maintain financial stability, systems often respond by increasing productivity expectations. Physicians are asked to see more patients, generate more wRVUs, and improve throughput.
The result? Higher workload without proportional financial recognition.
This creates a difficult situation. Physicians want to provide thoughtful, patient-centered care but are operating in an environment that increasingly rewards volume and “efficiency”.
What This Means for Patient Care
When reimbursement pressure limits resources, practices may struggle to hire adequate support staff or additional faculty. Appointment availability and OR time shrink. Anesthesiologists are asked to work more, take more call, give up vacation, accept lower reimbursement. Physicians get tired and increased locum personnel are brought in, which can disrupt an already strained work environment. Independent practices may consolidate or close, reducing local access and continuity.
A Sustainable Future Requires Balance
Physicians are asking for balance and sustainable practices— for competitive insurance markets that allow fair negotiation, and for reimbursement structures that reflect the complexity and intensity of modern clinical work.
Robust competition in insurance markets benefits patients and physicians alike.
Physicians want to continue practicing anesthesiology in a way that is safe, fulfilling, and that prioritizes patient safety. That requires financial models to support multiple practice models, including independent practice, working with trainees, caring for the sickest patients, not just rewarding volume at the expense of value.
The pressures are real. The data are clear. Burnout is increasing.
Supporting physician sustainability is not self-serving — it is foundational to maintaining access, quality, and trust in the health care system.

References
- American Medical Association. (2024). How health insurance consolidation hurts patients and physicians. Retrieved from https://www.ama-assn.org/health-care-advocacy/access-care/how-health-insurance-consolidation-hurts-patients-physicians
- Becker’s Hospital Review. (2024). The physician work-pay gap widens. Retrieved from https://www.beckershospitalreview.com/compensation-issues/the-physician-work-pay-gap-widens/
- Chernov M. Private Equity and Anesthesia Systems: Balancing Market Efficiency With Clinical Continuity. Anesth Analg. Published online March 5, 2026. doi:10.1213/ANE.0000000000008010
- Xie K, Robinson CL, Yong RJ. Reviewing Current Trends: Private Equity in Anesthesiology. Anesthesiology 2026, Feb 13. doi: 10.1097/ALN.0000000000005918. Epub ahead of print. PMID: 41685772.

